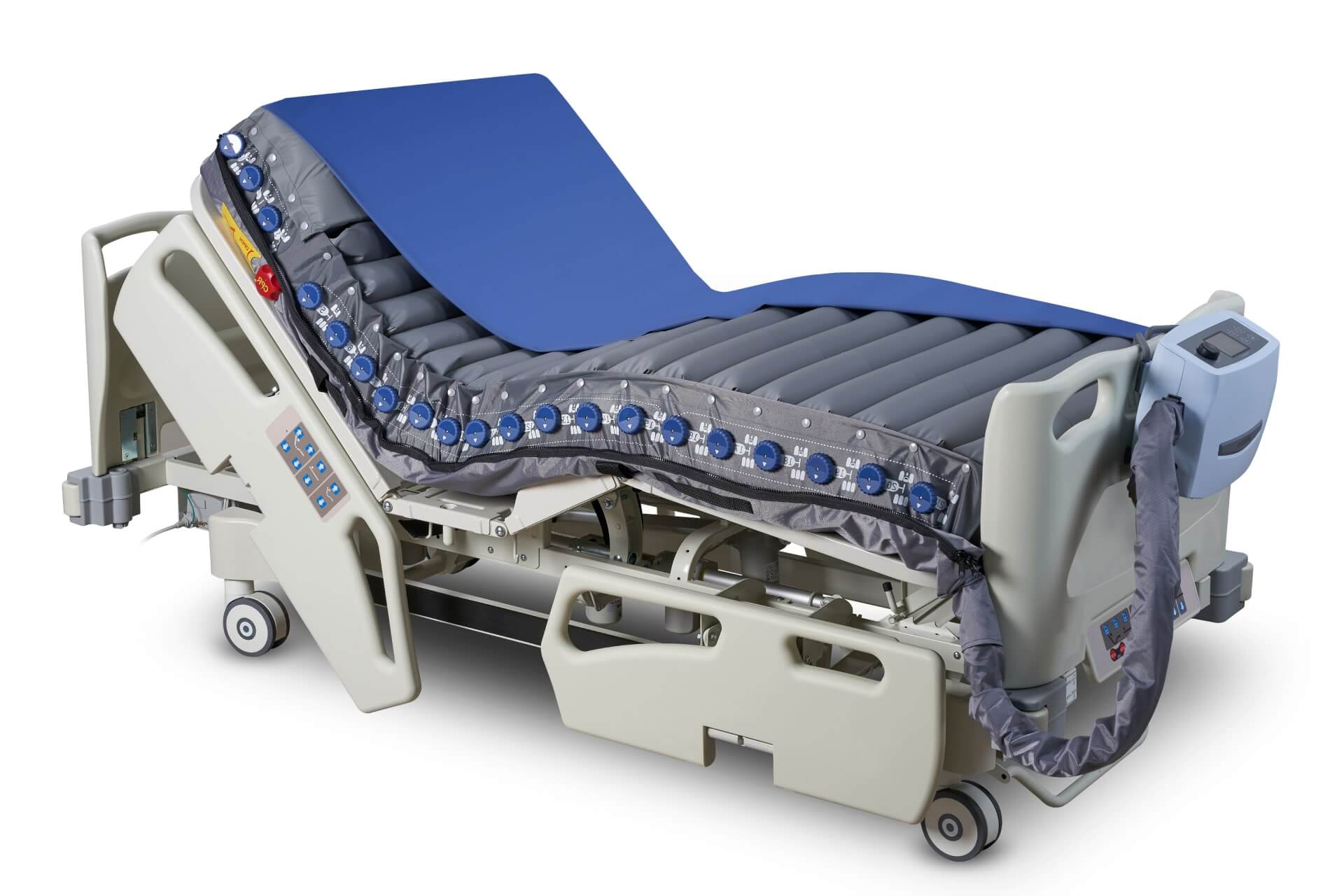
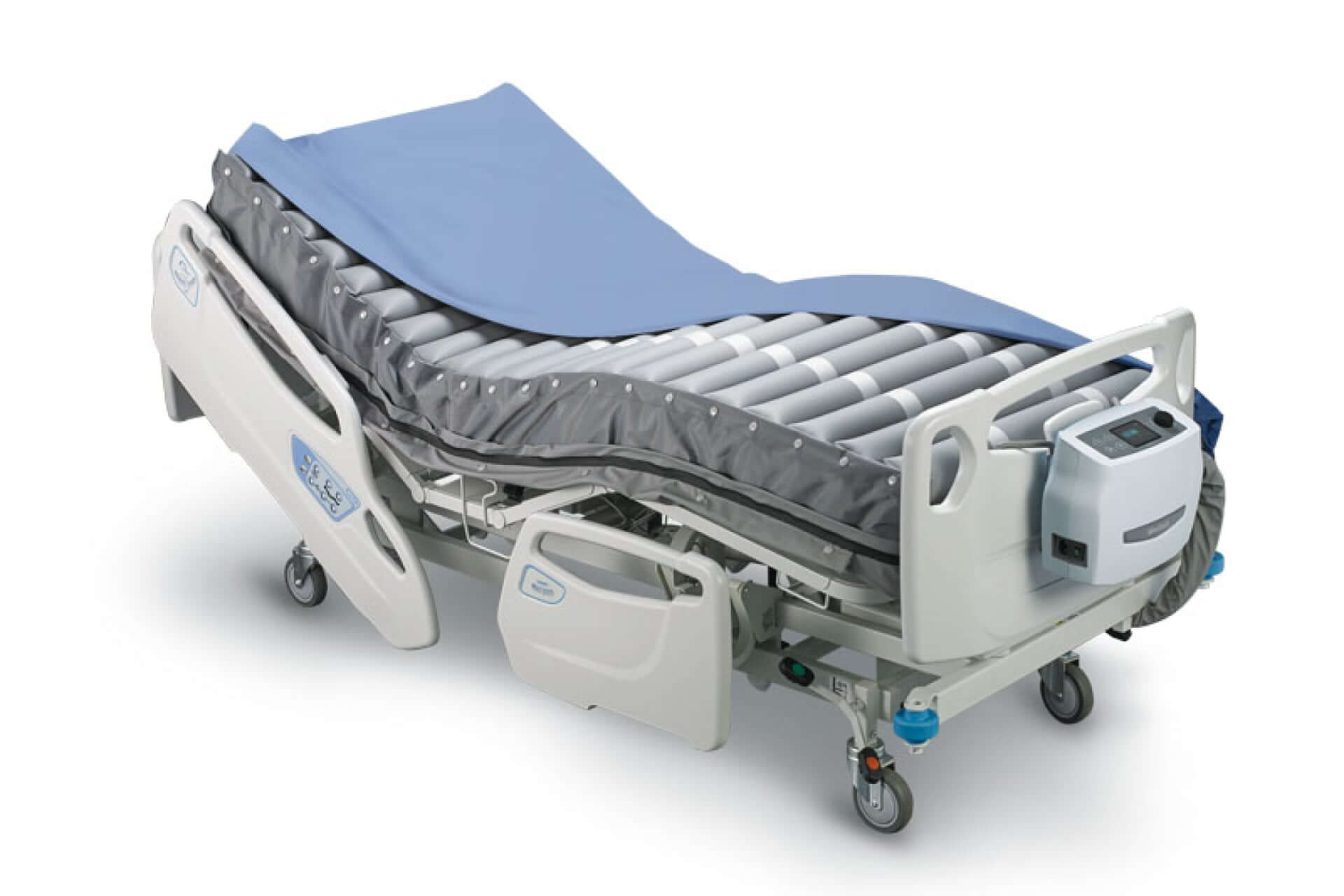
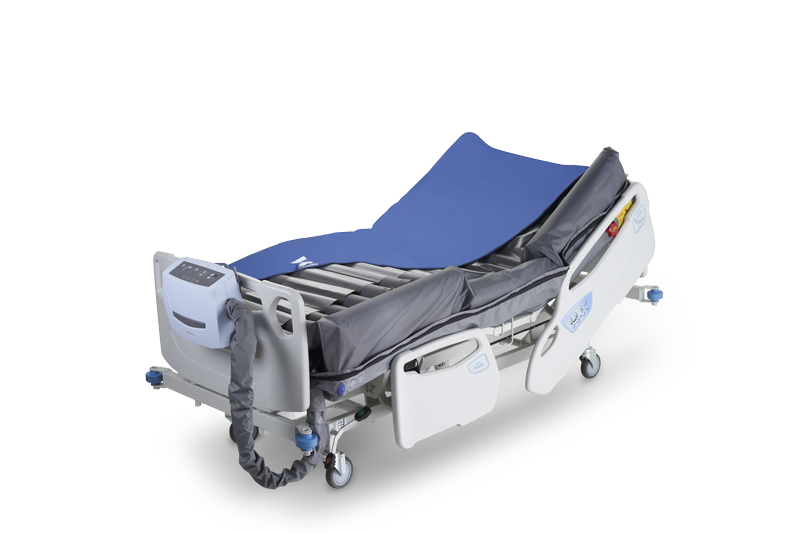
Optima Prone
Automating prone shoulder lifting and full-body pressure relief — Reducing workflow complexity and pressure injury risks.
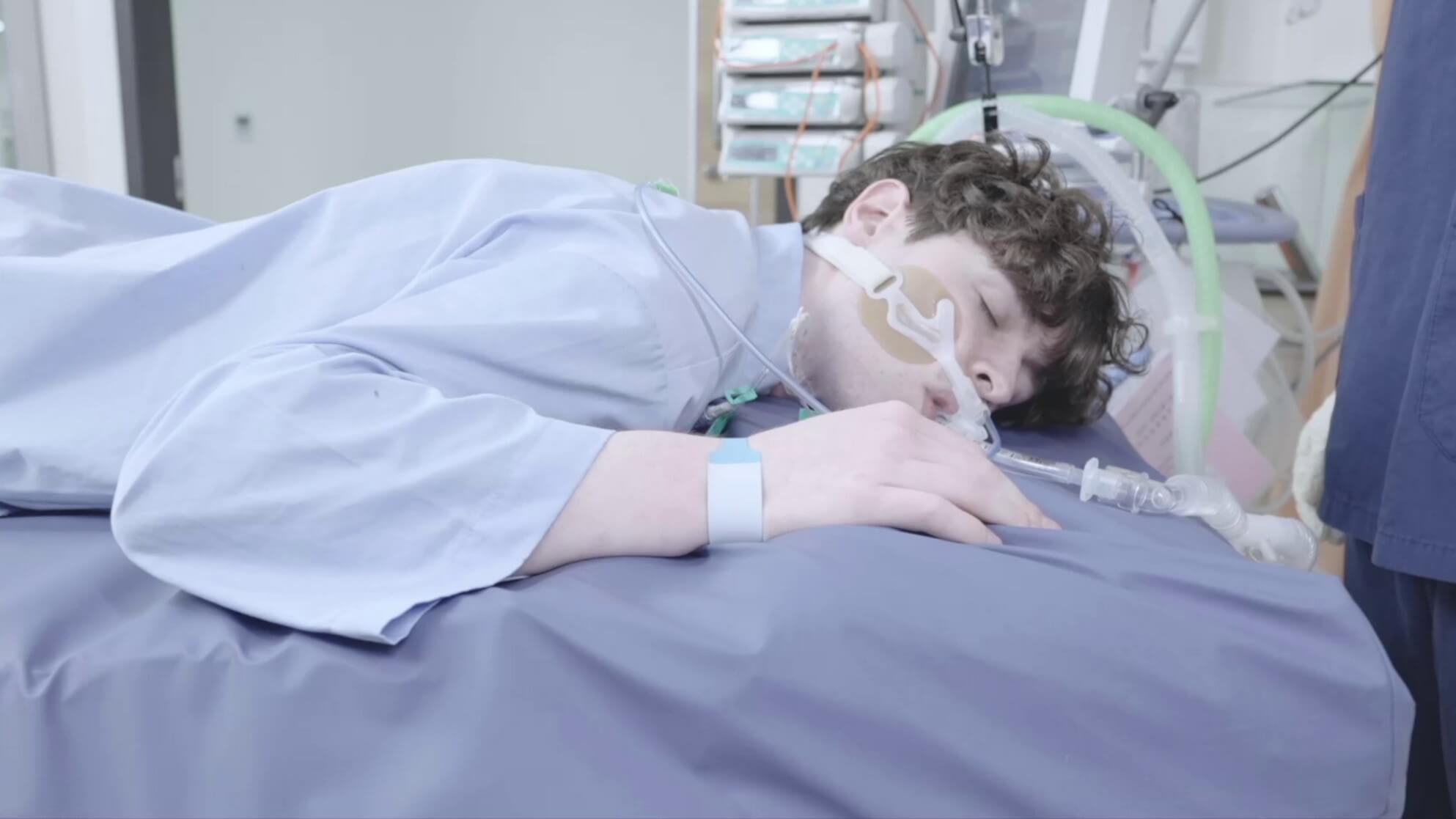
A staggering 75% of COVID-19 ICU patients require intensive treatments for severe respiratory distress involving mechanical breathing support.1 The 74% mortality rate from severe respiratory distress-associated COVID-19 cases2 overwhelms global healthcare systems, leading to a devastating shortage of resources and imposing complexity and burden on intensive care units and prone positioning therapy management.
Proned and intubated COVID-19 patients undergo prone treatments for an average of 5 hospital days. However, as proning results in a higher risk of developing pressure injuries (PI), these patients may require 3 more hospital days to treat PI-related complications3,4, reducing the nurse-to-patient ratio further.5
Optima Prone's head-to-toe pressure alternation, mechanical apparatus for assisting single-caregiver head repositioning, personalized pressure care with individual air cell deflation, and a unique facial pillow with sculpted ear pocket reduces caregiver workload and risks of pressure injuries, improving patient outcomes.

Simplify Head Repositioning
Mechanically supporting shoulder lifts while creating space below the patient's chin decreases the caregiver's workload and risk of obstructing airway tubing, allowing the single-caregiver to perform head repositioning safely and efficiently.
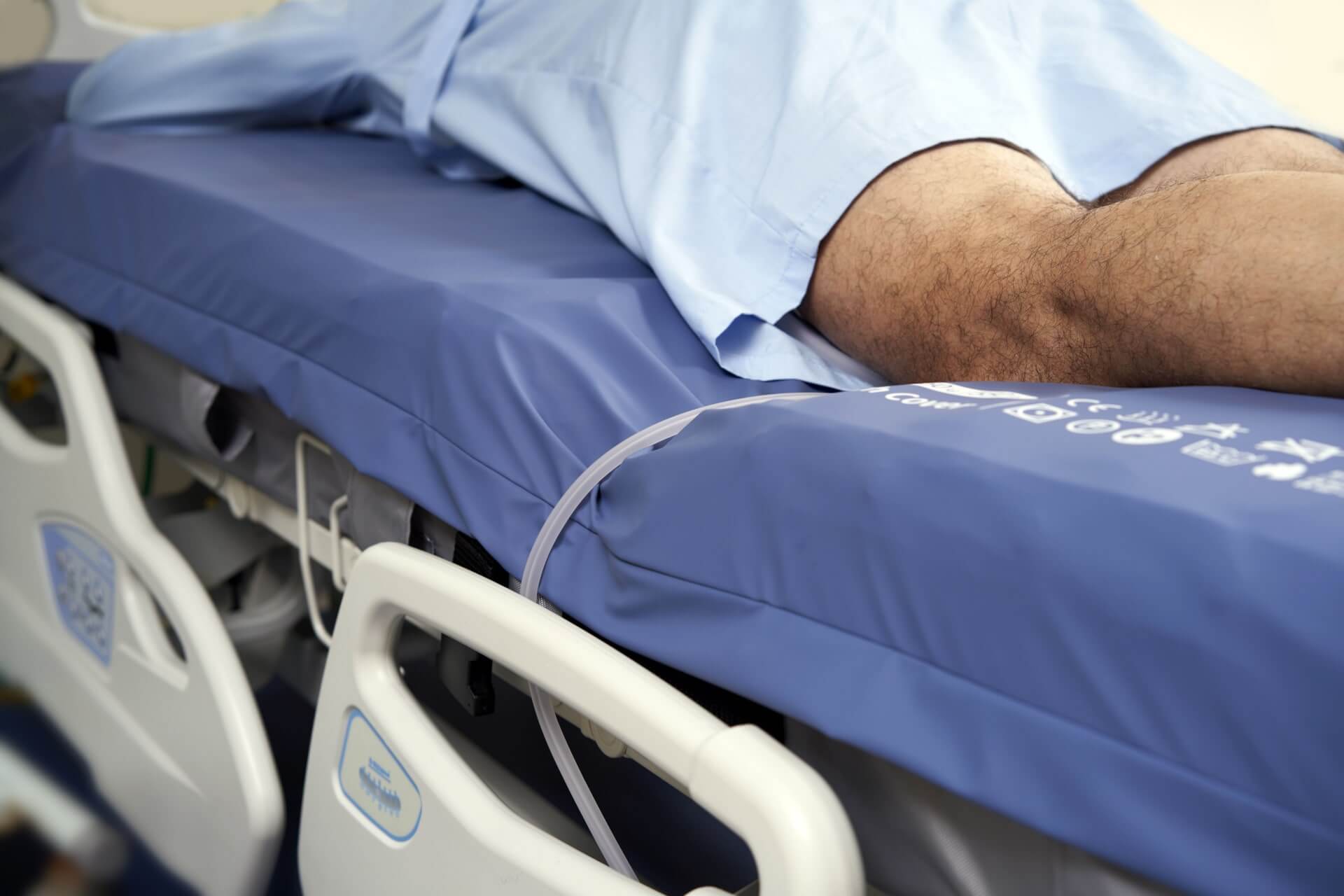
Manage Airway & Fluid Tubing
Deflating individual air cells to guide proper airway and fluid tubing organization prevents potential obstructions or displacements to hemodialysis flow and catheters, reducing the burden on the caregiver's workflow.

Prevent Pressure Injury Risks
Combining a unique headrest (facial pillow, sculpted ear pocket, and alternation pressure), a personalized pressure care system (individual air cell deflation), and cell airflow tracking prevents pressure injury risks, improving patient outcomes.
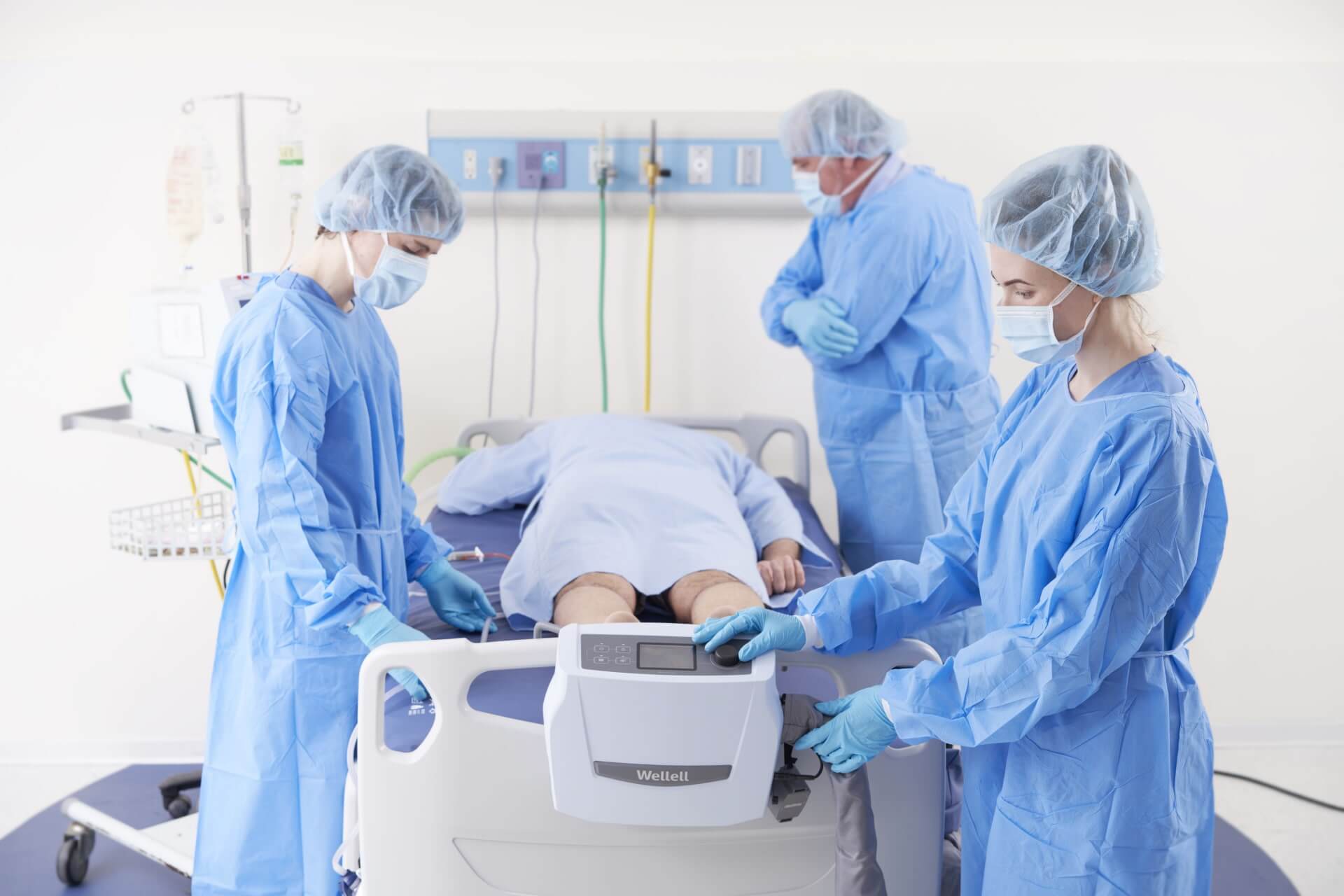
Access to Controls via Interface
Visual interface with LCD enables quick access to controls such as alternating and zone pressure settings, therapy timer, shoulder lift apparatus, and alarm system settings, simplifying patient care for caregiver across all experience levels.
| Standard 200 | ||
|---|---|---|
| Mattress Dimension | 78.7 x 35.4 x 5 in, with side bolster 10 in | 2000 x 900 x 130 mm, with side bolster 254 mm |
| Mattress Weight | 27.5 lb | 12.5 kg |
| Maximum Patient Weight | 397 lb | 180 kg |
| Narrow 200 | ||
|---|---|---|
| Mattress Dimension | 78.7 x 33.5 x 5 in, with side bolster 10 in | 2000 x 850 x 130 mm, with side bolster 254 mm |
| Mattress Weight | 27.5 lb | 12.5 kg |
| Maximum Patient Weight | 397 lb | 180 kg |

Simplify Head Repositioning
Mechanically supporting shoulder lifts while creating space below the patient's chin decreases the caregiver's workload and risk of obstructing airway tubing, allowing the single-caregiver to perform head repositioning safely and efficiently.

Manage Airway & Fluid Tubing
Deflating individual air cells to guide proper airway and fluid tubing organization prevents potential obstructions or displacements to hemodialysis flow and catheters, reducing the burden on the caregiver's workflow.

Prevent Pressure Injury Risks
Combining a unique headrest (facial pillow, sculpted ear pocket, and alternation pressure), a personalized pressure care system (individual air cell deflation), and cell airflow tracking prevents pressure injury risks, improving patient outcomes.

Access to Controls via Interface
Visual interface with LCD enables quick access to controls such as alternating and zone pressure settings, therapy timer, shoulder lift apparatus, and alarm system settings, simplifying patient care for caregiver across all experience levels.
Reducing prone procedure complexity and caregivers’ workload, and improving patient care and outcome.
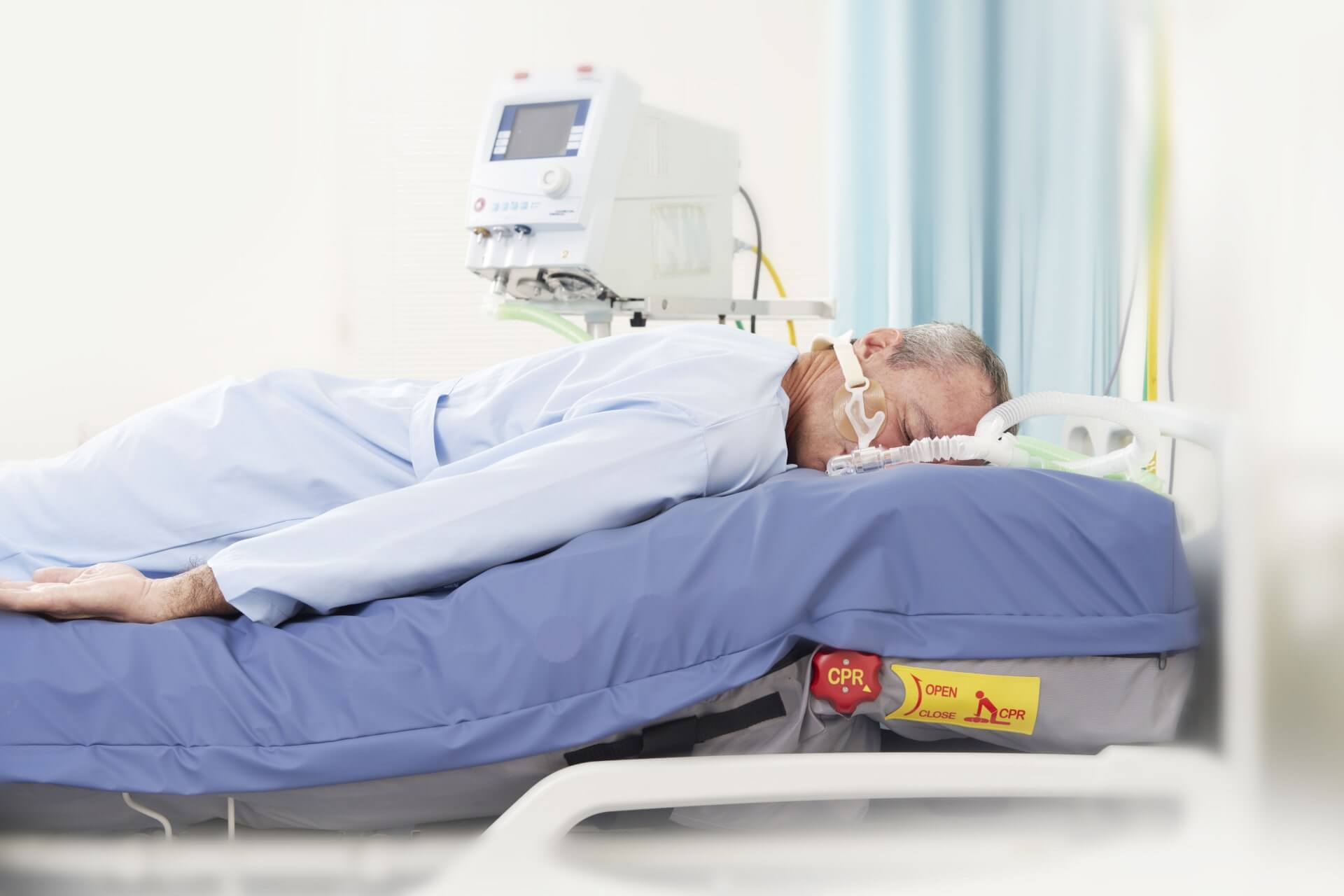
Proning reduces intubation and mortality rate for ARDS.
Early prolonged prone-positioning treatment for respiratory-distressed patients improves blood oxygenation (PaO2/FiO2 ratio), prevents further complications, and reduces mortality rate, acute care admissions, and in-hospital days.6,7
No. During this time, the Automatic Pressure Adjustment is inactive and will not be detecting the patient's weight.
Deflation should follow the location of the patient's vulnerable areas. Our recommendations are:
- Head section (supine): 1 cell between cell No. 1 to No. 3
- Head section (prone): All cells between cell No. 1 to No. 3
- Torso section: 2 cells between cell No. 5 to No. 15
- Lower leg section: 1 cell between cell No. 16 to No. 21
The Shoulder Lifting Mode activates a mechanical apparatus that lifts and holds the patient's shoulders and chest upward, mimicking traditional prone positioning therapy's manual shoulder lifting procedure done by two or more caregivers. The lift helps release neck pressure that often leads to hyperextension injury and avoid spinal deformity body pains.
Caregivers have 10 minutes to reposition the patient's head while the mechanical apparatus assists in lifting the shoulders and chest upward. After 10 minutes, the mode automatically deactivates and returns to initial settings. Caregivers can cancel anytime during the procedure through the pump's interface.
In addition to lifting and supporting the patient's shoulder and chest upwards, the Shoulder Lifting Mode also deflates the area below the patient's chin, creating space for the caregiver to secure a steady hold and turn the head while safely managing and preventing airway tubing obstructions.
Yes. Alternating pressure will automatically take over once the Supine Position Mode or Prone Position Mode deactivates after 20 minutes of operation.
Aside from deflating individual cells to relieve pressure on the patient's vulnerable areas, caregivers can do the same but, with less intensity, for other body parts like the abdominal area, which is often protruding and easy to experience discomfort.
Optima Prone's Transport Mode refers to the combination of:
- An optional battery pack that provides non-stop alternating pressure relief for up to 6 hours and,
- The standard 24-hour Wellell mattresses stay inflated (if individual air cells are not adjusted).
All air cells are made from Thermoplastic Polyurethanes (TPU). It is highly resistant to breaking down when in contact with water (hydrolysis), soft to touch, and minimizes friction and noise during patient movements.
Cell-in-cell design refers to encapsulating a firm air cell within a larger outer cell, doubling the effect of firmness and stability for patients. Wellell’s Optima Series, including Prone, uses air cells with the cell-in-cell design in the sacrum area to improve patient support and comfort during sitting positions and when patients leave and enter the bed.
Reference
- Potere, Nicola et al. “Acute complications and mortality in hospitalized patients with coronavirus disease 2019: a systematic review and meta-analysis.” Critical care (London, England) vol. 24,1 389. 2 Jul. 2020, doi:10.1186/s13054-020-03022-1
- Yang, Xiaobo et al. “Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study.” The Lancet. Respiratory medicine vol. 8,5 (2020): 475-481. doi:10.1016/S2213-2600(20)30079-5
- Shearer, Sarah C et al. “Facial Pressure Injuries from Prone Positioning in the COVID-19 Era.” The Laryngoscope vol. 131,7 (2021): E2139-E2142. doi:10.1002/lary.29374
- Douglas, Ivor S et al. “Safety and Outcomes of Prolonged Usual Care Prone Position Mechanical Ventilation to Treat Acute Coronavirus Disease 2019 Hypoxemic Respiratory Failure.” Critical care medicine vol. 49,3 (2021): 490-502. doi:10.1097/CCM.0000000000004818
- da Silva Neto, Raimundo Monteiro et al. “Psychological effects caused by the COVID-19 pandemic in health professionals: A systematic review with meta-analysis.” Progress in neuro-psychopharmacology & biological psychiatry vol. 104 (2021): 110062. doi:10.1016/j.pnpbp.2020.110062
- Coppo, Anna et al. “Feasibility and physiological effects of prone positioning in non-intubated patients with acute respiratory failure due to COVID-19 (PRON-COVID): a prospective cohort study.” The Lancet. Respiratory medicine vol. 8,8 (2020): 765-774. doi:10.1016/S2213-2600(20)30268-X
- Guérin, Claude et al. “Prone positioning in severe acute respiratory distress syndrome.” The New England journal of medicine vol. 368,23 (2013): 2159-68. doi:10.1056/NEJMoa1214103